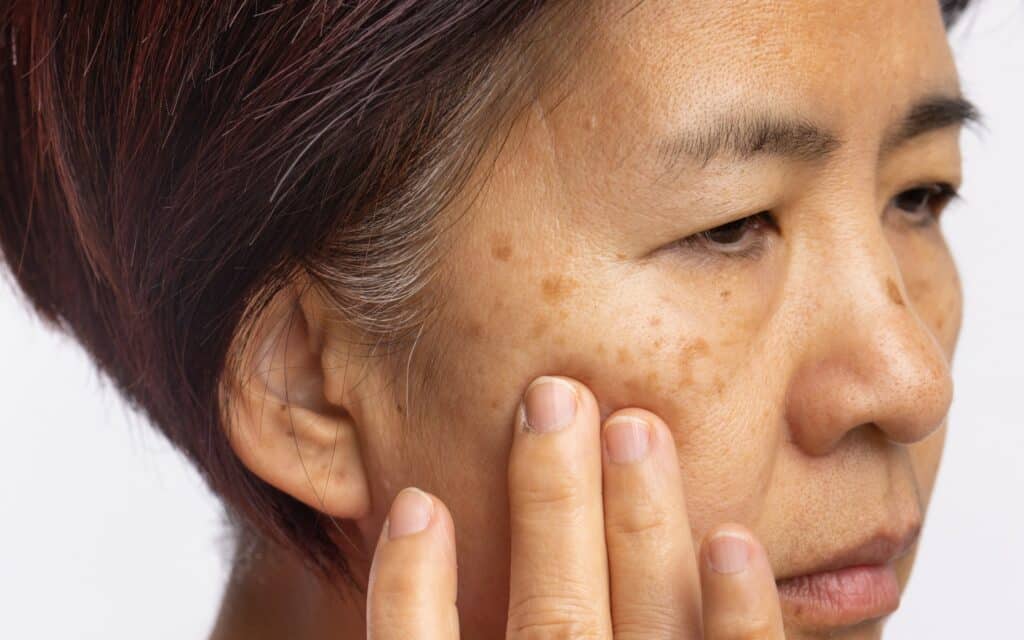
Welcome to The Derm Spot, your trusted source for dermatology and skin care advice. If you’ve ever stared at a patch of stubborn pigment and wondered, “Is this melasma vs sun spots, and does it change how I treat it?”, you’re in the right place. Getting this call right matters: melasma and sun spots look similar at a glance, but they form differently, respond to different treatments, and behave differently over time. In this guide, you’ll learn how to tell them apart at home, when to see a dermatologist, and which 2026 treatment options actually deliver clearer, more even-toned skin.
What Melasma Is vs Sun Spots: How They Form
Causes and Triggers
• Melasma: A chronic pigmentary condition driven by multiple factors, UV and visible light exposure, hormones (pregnancy, oral contraceptives, hormone therapy), heat, and genetic predisposition. In melasma, melanocytes are hypersensitive and overproduce melanin: there’s also increased vascularity and inflammation, which is why it rebounds easily.
• Sun spots (solar lentigines): Discrete, UV-induced lesions caused by cumulative sun exposure. Think of them as souvenir stamps from years of outdoor time. They’re not hormone-driven, and they don’t tend to be as reactive as melasma once removed, provided you protect your skin.
Who Is Most Affected
• Melasma: More common if you have medium to deeper skin tones (Fitzpatrick III–VI), a family history, or hormonal shifts (pregnancy, OCPs). It’s more frequent in women but can affect men.
• Sun spots: Show up across all skin tones with age and sun exposure, especially if you burn easily (Fitzpatrick I–III). They often accumulate after decades of outdoor activity.
Where They Appear and How They Look
• Melasma: Usually symmetric and patchy on the face, cheeks, upper lip, forehead, chin. The borders are soft/blurred. Color ranges from light to dark brown, sometimes with a gray-brown cast.
• Sun spots: Small, well-defined macules or flat patches on high-UV areas, face, hands, shoulders, arms, chest. They’re usually isolated or in clusters rather than broad patches and tend to be tan to medium brown with crisp edges.
How To Tell Melasma From Sun Spots at Home
Pattern, Symmetry, and Color Clues
Use a simple checklist:
- Distribution: Symmetric patches on cheeks/forehead/upper lip suggest melasma: scattered, individual spots with sharp borders suggest sun spots.
- Edge quality: Fuzzy edges → melasma. Crisp, ink-drop edges → sun spot.
- Tone: Gray-brown or mixed brown → melasma: uniform tan-to-brown → sun spot.
- Size: Patches that merge → melasma: coin-like dots or ovals → sun spots.
Bonus cue: Makeup behavior. Melasma often shows through sheer coverage as a shadow: sun spots are easier to spot-conceal.
What Worsens or Improves Each
• Melasma worsens with sun, visible light (including some indoor lighting), heat (saunas, hot yoga), friction, and hormonal changes. It may improve with strict photoprotection, tinted sunscreen, gentle actives (azelaic acid, tranexamic acid), and patience.
• Sun spots deepen with unprotected UV exposure. They improve with retinoids, exfoliating acids, and device-based removal (IPL, lasers), plus diligent sunscreen to prevent re-darkening.
If your “melasma vs sun spots” guess shifts because heat or hormones change the pigment, you’re likely dealing with melasma.
Diagnosis and When To See a Dermatologist
Wood’s Lamp, Dermoscopy, and Fitzpatrick Type
A board-certified dermatologist can refine the diagnosis:
• Wood’s lamp exam: May highlight epidermal melanin (often more responsive to topicals). Dermal-predominant melasma appears less enhanced and is tougher to treat.
• Dermoscopy: Melasma shows a pseudo-network with indistinct borders: sun spots reveal sharply demarcated pigment networks or fingerprint-like patterns.
• Fitzpatrick type: Your baseline skin reactivity to sun helps guide safe treatment intensity and device choice, minimizing risk of post-inflammatory hyperpigmentation (PIH).
Conditions That Can Mimic Both
• Post-inflammatory hyperpigmentation (PIH) after acne, eczema, or procedures
• Drug-induced hyperpigmentation (e.g., minocycline, amiodarone)
• Lichen planus pigmentosus, Riehl’s melanosis
• Early seborrheic keratoses or pigmented actinic keratoses
See a dermatologist promptly if lesions are asymmetrical, have multiple colors (especially black/blue/red), change rapidly, or look different from your other spots. When in doubt, get it checked. You’ll find more on evaluation pathways in our Dermatology and Skin Health hubs: Dermatology and Skin Health.
2026 Treatment Options: What Works for Melasma
Melasma is treatable, but it’s a marathon, not a sprint. Your plan should reduce pigment production, calm inflammation, and protect against UV and visible light, while avoiding aggressive triggers that cause rebound.
Daily Skincare Actives (Azelaic Acid, Tranexamic Acid, Tretinoin)
• Azelaic acid 10–20%: Melanocyte-modulating and anti-inflammatory: well-tolerated for daily use.
• Tranexamic acid (topical or serum): Helps interrupt pigment signaling: pairs well with niacinamide and antioxidants.
• Tretinoin or retinaldehyde: Speeds cell turnover to lift surface pigment: start low and slow to avoid irritation.
• Support team: Niacinamide, vitamin C (stable forms), licorice extract, cysteamine (night treatments), and gentle AHA/BHA a few times weekly if your skin tolerates it.
• Sunscreen is non-negotiable: Broad-spectrum SPF 30–50+, ideally tinted to block visible light (iron oxides). Reapply every 2 hours outdoors.
Explore ingredient profiles in our A–Z library: Skincare Ingredients A to Z.
In-Office Procedures (Chemical Peels, Low-Fluence Lasers, Microneedling)
• Chemical peels: Supervised, low-to-medium strength glycolic, lactic, salicylic, or blended peels can lift epidermal pigment. Spacing and prep matter to avoid PIH.
• Low-fluence lasers: Subthermolytic approaches (e.g., low-fluence Q-switched or picosecond lasers) can help, but require expert hands and conservative settings to prevent rebound.
• Microneedling (with topicals): Can enhance penetration of lighteners and improve texture: avoid if your skin is inflamed or very reactive.
• Combination therapy: Gentle stacking (e.g., azelaic + tretinoin + periodic peels) often outperforms a single tactic.
Hormonal and Oral Therapies (Tranexamic Acid, Contraceptive Considerations)
• Oral tranexamic acid: For select patients with recalcitrant melasma, short courses under medical supervision can be effective. Not for everyone, your clinician will screen for clotting risks and medication interactions.
• Hormonal review: If melasma flared with a specific contraceptive or HRT, discuss alternatives or non-hormonal methods with your clinician.
Avoiding Triggers and Recurrence Management
• Daily: Tinted sunscreen, wide-brim hats, sunglasses, shade-seeking.
• Heat: Limit saunas, hot yoga, and prolonged heat exposure: cool skin post-workout.
• Gentle routine: Avoid harsh scrubs or over-peeling that can inflame and darken skin.
• Maintenance: After clearing, continue a lighter version of your regimen (e.g., azelaic + niacinamide + tinted SPF). Melasma likes to resurface, maintenance keeps it quiet.
For procedure deep-dives and candid pros/cons, browse our Cosmetic Treatments section: Cosmetic Treatments.
2026 Treatment Options: What Works for Sun Spots
Sun spots usually respond faster than melasma because they’re discrete lesions without the same hormonal/vascular drivers.
Topical Lighteners and Retinoids
• Retinoids (tretinoin, adapalene, retinal): Promote turnover and fade superficial pigment while improving texture.
• Tyrosinase inhibitors: Azelaic acid, kojic acid, arbutin, licorice extract, cysteamine, stabilized vitamin C. Use consistently for 8–12+ weeks.
• Exfoliants: Glycolic or lactic acid a few nights weekly can brighten and help topicals penetrate.
Device-Based Treatments (IPL, Q-Switched, Picosecond, Fractional)
• Intense Pulsed Light (IPL): Great for clusters of sun spots and redness on fair-to-medium tones. Not ideal for very deep tones due to PIH risk.
• Q-switched and picosecond lasers: Target melanin precisely: suitable for individual spots. Picosecond platforms offer shorter pulses that can reduce downtime.
• Fractional lasers (non-ablative or ablative): Useful when sun spots coexist with texture and fine lines: more downtime, often better for lighter skin tones.
Device choice depends on your Fitzpatrick type, spot depth, and downtime tolerance, an in-person assessment prevents over-treatment and PIH.
Spot-Specific Care and Aftercare
• Before: Precondition with sunscreen and gentle retinoids (as advised) to optimize outcomes.
• After: Baby the area, bland cleanser, fragrance-free moisturizer, strict SPF, and no picking. Expect temporary darkening (a coffee-ground look) before flaking with IPL/laser.
• Maintenance: Continue sunscreen and nightly retinoid to keep new spots from forming.
Sun Protection and Prevention Strategies
Sunscreen Types and Tinted/PPD Considerations
• Filters: Choose broad-spectrum SPF 30–50+. Mineral (zinc/titanium) is reliable and well-tolerated: modern hybrids feel lighter.
• Tinted formulas: For melasma, tinted sunscreens with iron oxides add visible-light protection, key for stubborn recurrence.
• PPD/UVA: High UVA protection (often labeled as PA ratings or measured via PPD) helps prevent deep pigment stimulation.
• Reapplication: Every 2 hours outdoors: every 60–90 minutes if sweating or swimming. Don’t forget hands, ears, and hairline.
Visible Light, Heat, and Lifestyle Habits
• Shade-smart: Wide-brim hats (UPF), UV-blocking sunglasses, and sun-protective clothing raise your “protection ceiling.”
• Indoors counts: Bright windows and screens add up, apply a morning layer daily.
• Heat management: Cool rinses post-workout, avoid steaming hot water on the face.
• Antioxidants: Vitamin C, E, ferulic, and niacinamide help buffer UV/oxidative stress when layered under SPF.
Explore more prevention insights in Skin Health and seasonal guides within Body Care.
Conclusion
When you’re weighing melasma vs sun spots, pattern and behavior tell the story: melasma forms symmetric, blurry patches that react to light, heat, and hormones: sun spots are crisp, discrete souvenirs of UV. That distinction guides treatment in 2026, gentle, multi-pronged maintenance for melasma vs targeted devices and spot care for sun spots. Start with strict daily photoprotection, layer proven actives, and consider in-office options tailored to your skin tone. If you’re unsure, or if pigment changes quickly, book a professional evaluation. With a precise diagnosis and a steady plan, clear, even-toned skin is absolutely within reach.
Melasma vs Sun Spots: FAQs
What is the key difference between melasma vs sun spots?
Melasma is a chronic, hormone- and light-sensitive condition that appears as symmetric, blurry patches on the face and often rebounds. Sun spots (solar lentigines) are discrete, UV-induced lesions with crisp edges on high-sun areas. They’re not hormone-driven and usually respond faster to spot treatments and devices.
How can I tell melasma from sun spots at home?
Check pattern, edges, and color. Melasma forms symmetric patches with soft borders and gray-brown or mixed tones, often on cheeks, forehead, and upper lip. Sun spots are individual tan-to-brown macules with sharp, “ink-drop” edges on face, hands, shoulders. Melasma also tends to show through makeup as a shadow.
What are the best 2026 treatment options for melasma?
Use a gentle, multi-pronged plan: daily tinted broad-spectrum SPF 30–50+, azelaic acid, topical tranexamic acid, and retinoids like tretinoin started slowly. Consider supervised chemical peels and low-fluence lasers in expert hands. Address triggers—heat, visible light, and hormones—and maintain results with ongoing sun protection and a simplified maintenance routine.
Is IPL or laser better for treating sun spots in 2026?
For sun spots, IPL works well for clusters on fair-to-medium tones, while Q‑switched or picosecond lasers precisely target individual spots. Fractional lasers help when texture and fine lines coexist. Device choice depends on skin tone (Fitzpatrick type), spot depth, and downtime tolerance—an in-person assessment minimizes PIH risk.
Can I use hydroquinone for melasma vs sun spots? (External)
Hydroquinone can fade both when used short-term under dermatology guidance, but it’s not ideal for long-term melasma maintenance due to rebound risk and rare ochronosis with prolonged use. Many clinicians favor cyclic or combination regimens with azelaic acid, retinoids, cysteamine, or tranexamic acid plus strict tinted SPF for durability.
What melasma treatments are pregnancy-safe, and what should I avoid? (External)
In pregnancy, prioritize strict sun protection (tinted mineral SPF), UPF hats, and gentle actives like azelaic acid and niacinamide. Avoid retinoids, oral tranexamic acid, and typically hydroquinone unless specifically advised. Focus on maintenance; many cases improve postpartum, and stronger options can be reconsidered later with your clinician.