Welcome to The Derm Spot, your trusted source for dermatology and skin care advice. If melasma has left you second‑guessing every sunny day or new product, you’re not alone. Those patchy brown or gray‑brown spots, most often on your cheeks, forehead, upper lip, and chin, can be stubborn and emotionally draining. In this guide, you’ll learn exactly what melasma is, why it happens, and the most effective, dermatologist‑approved treatments and daily habits for 2026. The goal: help you protect your skin, improve discoloration, and keep relapses to a minimum, without wasting time on trends that don’t work.
What Is Melasma?
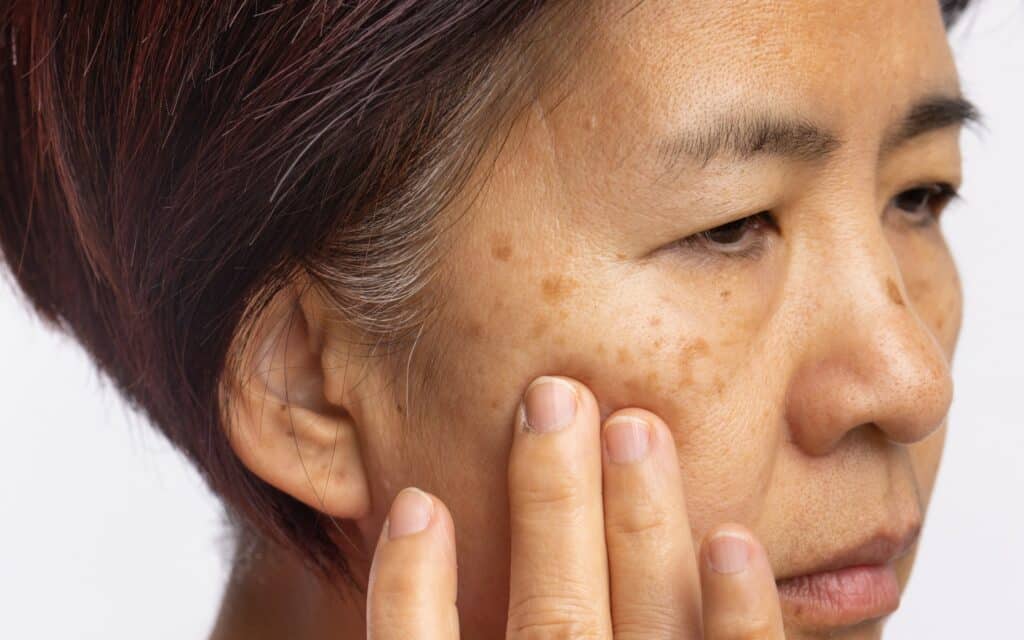
Melasma is a chronic pigmentary disorder that causes blotchy, symmetrical patches of hyperpigmentation on sun‑exposed areas, especially the face. It’s driven by excess melanin production in melanocytes and influenced by UV/visible light, heat, and hormones. While it’s not dangerous, melasma can be persistent, with flares that coincide with sun exposure, summer months, or hormonal shifts.
How Melasma Looks And Common Patterns
You typically see flat, irregularly shaped brown to gray‑brown patches with soft edges. The three classic distribution patterns are:
- Centrofacial: forehead, nose, cheeks, upper lip, and chin (most common)
- Malar: cheeks and nose
- Mandibular: jawline (less common and sometimes trickier to treat)
Color can hint at depth: light to dark brown suggests more epidermal involvement: gray or blue‑gray suggests deeper dermal pigment.
Who Is Most At Risk
- Women, especially during childbearing years (but men can develop melasma, too)
- Medium to darker skin tones (Fitzpatrick III–VI)
- People with a family history of melasma
- Those with significant sun or heat exposure (outdoor work, hot yoga, saunas)
- Individuals using hormonal contraception or undergoing fertility or hormone therapies
Causes And Triggers You Can Control
Melasma is multifactorial. You can’t control your genetics, but you can tackle the external triggers that drive flares and deepen pigmentation.
Sunlight, Visible Light, And Heat Exposure
- Ultraviolet (UVA/UVB) light stimulates melanocytes: even a few minutes daily adds up.
- Visible light, especially high‑energy blue light, can darken melasma, particularly in darker complexions.
- Heat (infrared, hot environments, steam facials) can worsen discoloration by promoting inflammation and vascular signaling.
Actionable moves:
- Use a high‑protection, broad‑spectrum sunscreen daily and reapply.
- Choose iron‑oxide–tinted formulas to block visible light.
- Seek shade, wear a wide‑brim hat, and avoid peak sun hours when you can.
- Limit unnecessary heat exposure (very hot workouts, saunas, steaming facials).
Hormonal Influences And Life Stages
- Pregnancy (“the mask of pregnancy”) and postpartum shifts
- Combined oral contraceptives or progestin‑only methods in some individuals
- Fertility treatments and hormone replacement therapy
If melasma appears after starting a hormonal method, talk to your clinician about alternatives. Never stop prescribed therapy without a medical discussion.
Medications, Cosmetics, And Skin Irritation
- Certain photosensitizing medications (some antibiotics, anti‑seizure drugs) can amplify UV effects.
- Fragrance, essential oils, and harsh exfoliants may irritate skin, causing post‑inflammatory pigment that blends with melasma.
- Inconsistent sunscreen use or skipping reapplication undermines progress.
Keep products gentle and fragrance‑free. Patch test new actives and avoid over‑exfoliating.
Diagnosis And Types
How Clinicians Confirm Melasma
A dermatologist typically diagnoses melasma by examining your skin and medical history. Tools that may be used:
- Wood’s lamp to estimate pigment depth (helpful but not foolproof)
- Dermoscopy to assess pigment network and vascular components
- In select cases, reflectance confocal microscopy (noninvasive imaging) for detailed evaluation
- Baseline photos and a scoring system (like MASI or mMASI) to track progress realistically over months
Patterns And Depth: Epidermal, Dermal, And Mixed
- Epidermal melasma: pigment sits more superficially, often responds faster to topicals and sun protection
- Dermal melasma: pigment is deeper, usually slower to improve and more relapse‑prone
- Mixed melasma: most common: requires layered strategies and long‑term maintenance
Depth guides expectations rather than dictating success. Consistency is still the biggest predictor of results.
Effective Treatment Options In 2026
Melasma management in 2026 focuses on multi‑pathway approaches: daily photoprotection, pigment‑modulating topicals, select oral therapy, and cautious procedures. Think marathon, not sprint.
Daily Photoprotection And Tinted Sunscreens
- Choose SPF 50+ broad‑spectrum sunscreen with high UVA protection (look for PA++++ or UVA circle ratings where available).
- Prioritize iron‑oxide–tinted mineral or hybrid sunscreens to block visible light. Apply a generous layer and reapply every 2 hours outdoors.
- Add physical barriers: UPF hats, sunglasses, and shade. Every bit reduces cumulative exposure.
- Consider oral adjuncts like Polypodium leucotomos extracts for UV defense. They’re not a substitute for sunscreen, but can be a helpful add‑on.
Medications: Topicals And Oral Tranexamic Acid
Well‑studied topical options for melasma include:
- Triple‑combination cream: hydroquinone (usually 4%), tretinoin, and a mild corticosteroid in intermittent courses (e.g., 8–12 weeks) under medical guidance
- Non‑hydroquinone brighteners for long‑term use or maintenance: azelaic acid 15–20%, kojic acid, arbutin, niacinamide, cysteamine, licorice extract, and newer tyrosinase or melanogenesis inhibitors
- Topical tranexamic acid (2–5%) can support tone evening, especially in maintenance phases
Oral tranexamic acid (TXA):
- Low‑dose oral TXA (commonly 250 mg twice daily) is widely used off‑label for moderate to severe melasma.
- Benefits: can reduce stubborn pigmentation and relapse frequency, especially when combined with sunscreen and topicals.
- Safety: generally well‑tolerated, but not for everyone. It’s contraindicated in people with a history of thromboembolic disease, certain clotting disorders, or on some hormonal regimens. You’ll need a personalized risk assessment and monitoring with your dermatologist.
Procedures And Devices Used With Caution
Procedures can help, but only when your daily routine is rock‑solid and skin is stable.
- Chemical peels: very superficial glycolic, lactic, mandelic, or Jessner’s peels at conservative strengths and intervals. Pre‑ and post‑peel sun protection is non‑negotiable.
- Lasers and light devices: low‑fluence, pigment‑safe protocols (e.g., 730 nm picosecond devices, low‑energy 1064 nm QS/PS, or fractional 1927 nm thulium) may help selected patients. Over‑aggressive settings risk rebound hyperpigmentation.
- Microneedling with topical delivery (e.g., tranexamic acid) is an option in trained hands, again with strict photoprotection.
Golden rule: treating melasma with energy devices demands conservative parameters, spacing, and maintenance topicals to prevent rebound. If a clinic promises “one‑and‑done” results, be skeptical.
For more on in‑office options, explore our updates in cosmetic treatments.
Daily Care, Prevention, And Realistic Expectations
A Simple Morning-And-Night Routine
Keep it consistent and gentle:
Morning
- Cleanse: mild, fragrance‑free cleanser
- Treat: antioxidant serum (vitamin C or ferulic‑supported blends) if tolerated
- Protect: iron‑oxide–tinted SPF 50+: finish with hat/sunglasses for outdoor time
- Optional: mineral makeup with added iron oxides for visible‑light defense
Night
- Cleanse
- Treat: your dermatologist‑directed therapy, e.g., azelaic acid or triple‑combination cream in cycles: on off nights, consider niacinamide or a barrier‑support moisturizer
- Moisturize: barrier‑repair cream with ceramides, glycerin, and cholesterol
Sensitive to retinoids? Start twice weekly and build up, or use azelaic acid as your primary evening active. For more ingredient deep dives, visit our Skincare Ingredients A‑to‑Z.
Maintenance To Reduce Relapse
- Stick with tinted sunscreen every single morning, all year.
- Continue a non‑hydroquinone brightening regimen (azelaic acid, cysteamine, kojic acid, niacinamide) for long‑term use.
- Consider seasonal strategies: intensify topicals in spring/summer, taper peels and devices to cooler months.
- Track triggers: heat exposure, high‑UV trips, and inconsistent reapplication are common culprits.
- Plan for touch‑ups: melasma relapses are common: quick intervention prevents backsliding.
When To See A Dermatology Professional
- You’re unsure if it’s melasma vs. another pigment condition (e.g., post‑inflammatory hyperpigmentation, drug‑induced pigmentation, lichen planus pigmentosus)
- Over‑the‑counter brighteners haven’t helped after 8–12 weeks
- You’re considering oral tranexamic acid, peels, lasers, or microneedling
- You’ve developed irritation, redness, or worsening patches on current products
A board‑certified dermatologist can tailor a plan to your skin tone, lifestyle, and risk profile. If you’re curious about broader topics, browse our hubs on dermatology and skin health.
Conclusion
Melasma thrives on light and heat, and on inconsistency. Your best results come from a layered strategy: daily iron‑oxide–tinted SPF, smart brighteners, selective medical therapies like oral tranexamic acid when appropriate, and cautious procedures only after your routine is dialed in. Expect steady, incremental gains over weeks to months and plan for maintenance to outsmart relapses. With a clear plan and patient follow‑through, you can keep melasma in check and feel good in your skin, this year and beyond. For more practical guidance across face and body routines, explore our insights in skin health and body care.
Melasma: Frequently Asked Questions (2026)
What is melasma and what causes it?
Melasma is a chronic pigmentary disorder causing symmetrical brown or gray‑brown patches on sun‑exposed areas, especially the face. It’s driven by excess melanin from melanocytes and triggered by UV/visible light, heat, and hormones. Flares often coincide with summer, sun exposure, pregnancy, or hormonal contraception. It’s benign but persistent without consistent management.
What are the most effective melasma treatments in 2026?
Top results come from a layered plan: daily SPF 50+ broad‑spectrum, iron‑oxide–tinted sunscreen; gentle brighteners (azelaic acid, niacinamide, kojic acid, cysteamine); intermittent triple‑combination cream under supervision; and, in select cases, oral tranexamic acid. Conservative chemical peels or pigment‑safe laser protocols can help once skin is stable, always with strict photoprotection.
How long does melasma treatment take, and can it come back?
Expect gradual improvement over weeks to months, not days. Epidermal melasma tends to respond faster than dermal or mixed types. Relapses are common, especially with sun or heat exposure. Maintenance is key: daily tinted sunscreen, ongoing non‑hydroquinone brighteners, seasonal adjustments, and early “touch‑ups” if darkening starts to reappear.
What sunscreen is best for melasma?
Choose SPF 50+ broad‑spectrum with strong UVA protection (look for PA++++ or UVA‑circle ratings). Iron‑oxide–tinted mineral or hybrid formulas help block visible light that can darken melasma. Apply generously, reapply every two hours outdoors, and combine with UPF hats, sunglasses, shade, and heat‑management to reduce flares.
Which melasma treatments are safe during pregnancy or breastfeeding?
Focus on strict sun protection with iron‑oxide–tinted SPF and physical barriers. Azelaic acid is commonly considered a pregnancy‑safe brightener. Retinoids and hydroquinone are generally avoided during pregnancy. Procedural treatments are typically deferred. Always review any product or medication with your obstetrician and dermatologist before use.
Can diet or lifestyle changes improve melasma?
Diet alone won’t clear melasma, but supportive habits help. Manage heat exposure (avoid saunas, very hot workouts), practice rigorous photoprotection, and minimize skin irritation from fragrances or harsh exfoliants. A balanced diet with antioxidants supports overall skin health, but consistent sunscreen and targeted topicals drive the most visible results.